A frightening Torsade de Pointes happened during an event of intense chest pain, with a new dramatic electrocardiogram (ECG), remarkable for a striking ST elevation, later interpreted as a consensual depolarization variation, and dictated admission on September 23rd, 2023. During admission, ECG depolarization and repolarization variations were observed within the context of a new picture of severe left ventricular asymmetric hypertrophy, previously unknown. It was found phenotypically similar to hypertrophic cardiomyopathy, as also exhibited efflux obstruction, with pseudonecrosis Q waves, and marked consensual repolarization disturbances, as strikingly evident at the discharge electrocardiogram.

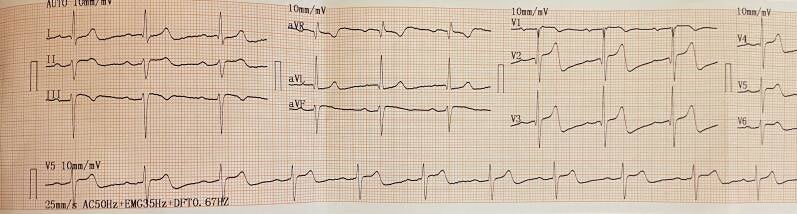
Torsade de Points ECG during chest pain, showing a classical appearance of hypertrophic cardiomyopathy

With the over-described stormy appearance of chest pain and life-threatening arrhythmias, the newly developed and reappraised asymmetric hypertrophic cardiomyopathy (HCM), with important dynamic obstruction to the outflow tract, quantified in 60 mmHg, made its tempestuous appearance on the scene. It happened at the age of 86 yrs, a really unusual and unexpected onset and finding for an HCM. Two, former by only 2 years, protracted hospital admissions during Sars-CoV-2 pandemics, had many times documented an important hypertensive burden and treatment, and accordingly, a left ventricular hypertrophy (a 14 mm-thick interventricular septum), without obstruction, up to the latest cardiac ultrasound, in October 2022.
Following the recent, upfront, and documented reappraisal of normal, for age, elderly hypertensive hypertrophy, the stormy admission on September 23rd, 2023, had disclosed unexpected data of a new asymmetric severe septal hypertrophy (26 mm), & a markedly varied electrocardiogram, consistent with an HCM picture. Due to the family epidemiology, what's more known to the daughter by only 12 days, but still not reported as of now, by hospital laboratories, all the data could then be reappraised to be indicative of a cysticercal cardiomyopathy.
Discharged on beta-adrenergic blockers, adjusted for the excessive initial dosing, a certain stability was achieved, with still persistent dyspnea on mild efforts. Later begun hyperbaric oxygen treatment, brought very remarkable betterments: reduced dyspnea, improved vascular health, and achieved, expected and documented at a later 2D Doppler ultrasound, taken on September 4th, 2025, strikingly reduced septal thickness (as compared with the recorded video support of the 2023 2D Doppler US), by at least 6-8 mm: the cysticercal infiltration was, as hypothesized, reduced by exposures to high, and hyperbaric, oxygen concentrations.
